Author: Matthew Wells, DO
Description
Unicameral Bone Cysts (UBC) — also called simple bone cysts — are benign (noncancerous) fluid-filled cavities that form inside bones. They are relatively rare in the general population, but when they do occur, they are almost always found in children and teenagers (typically between 3 and 17 years old).
UBCs most commonly develop in the proximal femur (near the hip, in the thigh bone) or the proximal humerus (near the shoulder, in the upper arm bone). These cysts can grow quite large and may thin the surrounding bone. When the bone becomes very thin, it can break easily, leading to what’s known as a pathologic fracture.
Doctors generally classify UBCs into two categories:
- Active: The cyst is still growing and may worsen or cause pain. This is more common when a child’s skeleton is still developing or when the cyst is located close to a growth plate.
- Latent: The cyst has matured and is unlikely to grow further or become more painful.
Symptoms
While some UBCs cause no pain and are discovered incidentally on X-rays, others can produce noticeable symptoms. Common symptoms include a dull, aching pain around the affected area and a limited range of motion in the nearby joint.
Because UBCs often occur in children and teenagers who are active in sports, the first sign of the cyst may be a pathologic fracture (a bone break that occurs through the cyst). In fact, studies show that up to two out of three patients with UBCs will experience a pathologic fracture at some point. Generally, cysts located in major weight-bearing bones of the lower extremity (like the thigh bone) are more likely to cause symptoms than those in non-weight-bearing bones of the upper extremity (like the upper arm bone).
Examination
Because unicameral bone cysts (UBCs) develop in the inside of the bone, they usually don’t cause obvious physical symptoms that can be seen or felt from the outside. Most patients only notice mild pain in the area. There are usually no rashes, skin changes, or major swelling. On exam, the area may be tender to touch, and movement of the nearby joint may be limited because of pain.
UBCs do not cause general symptoms such as fever, nausea, or vomiting. However, if a pathologic fracture (a break through the cyst) occurs, the symptoms are similar to those of any broken bone — sudden pain, swelling, and trouble walking or using the affected arm or leg.
Diagnostic Tests
Obtaining X-rays of the affected area is usually the first step in establishing the diagnosis of a UBC. A computed tomography (CT-scan) may be obtained to better characterize the UBC by your doctor if they feel it is needed for surgical planning. In some cases, UBCs can look like other tumors/cysts and your doctor may order an MRI to help confirm the diagnosis. A tissue biopsy is not typically needed to establish the diagnosis.
Images
On imaging, unicameral bone cysts (UBCs) are typically seen in the center of the bone, with thinning of the surrounding bone wall (cortex) (Figure 1). UBCs can grow large and cause the bone to expand, making it thin and weak. Sometimes, small pieces of bone can break off and fall into the cyst cavity — a feature known as the “fallen leaf sign” (Figure 2A).
On MRI scans, UBCs appear as fluid-filled cavities without any solid tissue or soft tissue mass around them (Figure 2B).
Figure 1. Anterior-posterior imaging of a minimally displaced pathologic fracture through a UBC found in the proximal humerus (A). UBCs can also arise in major weight bearing bones such as the proximal femur (B).
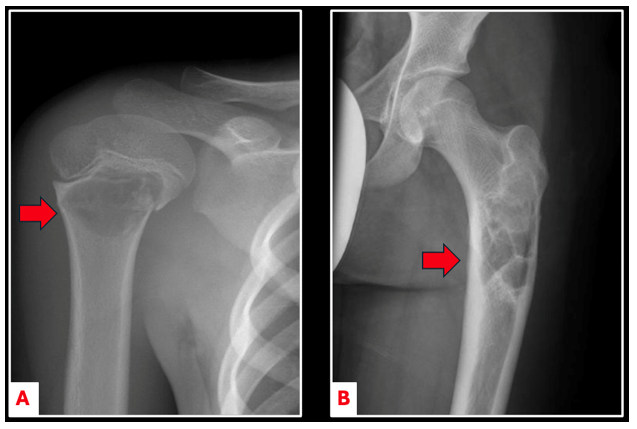
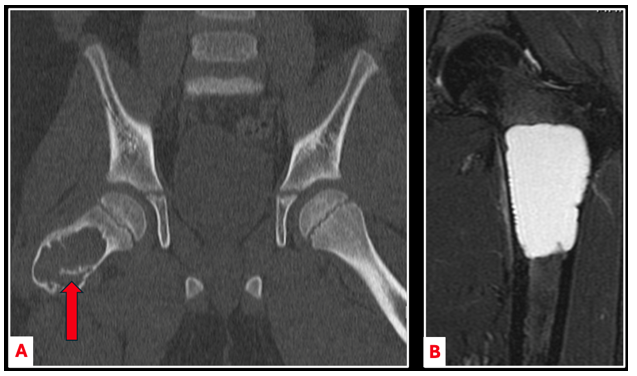
Figure 2. CT-scan imaging demonstrating the “fallen leaf sign” (red arrow) where a piece of bone fractures and falls into the cyst cavity (A). MRI-imaging demonstrating a large, fluid-filled cyst within the central aspect of a femur, consistent with a UBC (B).
Prognosis
Unicameral bone cysts (UBCs) have an excellent prognosis. Because they are benign (noncancerous), they do not spread to other parts of the body, and patients have a normal life expectancy. In many cases, especially when the cyst is small and not causing symptoms, it is perfectly reasonable to simply observe the cyst with follow-up imaging. However, UBCs can sometimes cause problems if the bone becomes weak and breaks through the cyst. This can be more serious if the fracture affects a growth plate in a child or teenager.
For that reason, doctors sometimes recommend treating a UBC before a fracture occurs. Smaller cysts in the arm or shoulder may be treated with minimally invasive procedures, such as injecting the cyst with corticosteroid, bone marrow, calcium sulfate, or other bone-forming materials to help it heal. Larger cysts, or those in weight-bearing bones like the hip, may require surgery to remove the cyst, fill the space with bone graft, and stabilize the bone for example with plate or screws (Figure 3).
Although the chance of the cyst coming back after treatment is low, recurrence is slightly more common in younger children (under 10 years old). For this reason, it is important to continue long-term follow-up with an orthopedic specialist. These patients are often cared for by orthopedic oncologists, who have expertise in the evaluation and treatment of bone and soft tissue tumors, including unicameral bone cysts.
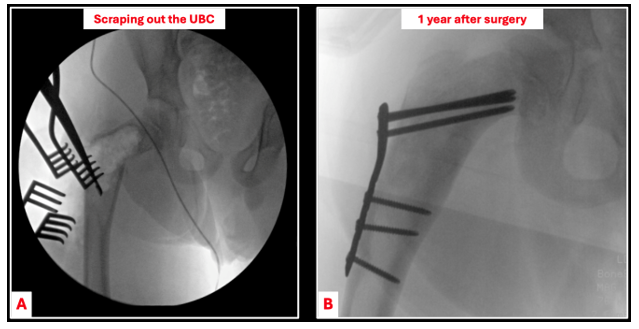
Figure 3. A 10-year-old boy presented with a proximal femur pathologic fracture through a UBC. He was treated with operative intervention involving scraping out the cyst (A) followed by placement of bone graft and plate/screw fixation during the same surgery. One year later, the cyst had resolved with successful bone healing (B) and the plate was removed.
More Information:
https://orthoinfo.aaos.org/en/diseases--conditions/unicameral-bone-cysts/
https://posna.org/physician-education/study-guide/unicameral-bone-cyst
This is not intended as a substitute for professional medical advice and does not provide advice on treatments or conditions for individual patients. All health and treatment decisions must be made in consultation with your physician(s), utilizing your specific medical information. Inclusion in this is not a recommendation of any product, treatment, physician or hospital.


